Журнал «Травма» Том 16, №3, 2015
Вернуться к номеру
Possibilities of telemedicine in work to improve survival in multiple trauma victims
Авторы: Guriev S.О., Fil А.Y. - Lviv national medical university name Danylo Galytskiy
Рубрики: Травматология и ортопедия
Разделы: Клинические исследования
Версия для печати
World experience providing medical assistance to victims of trauma indicates high efficiency of telemedicine methods in organization of medical care to trauma victims and an effective and adequate implementation of therapeutic and diagnostic measures. A condition of Ukraine’s health care system does not allow providing full medical and diagnostic care in all medical institutions of Ukraine. Therefore, there is request to continuing consulting practitioners with in damage control speciality, dynamics of treatment, as well as providing opportunities to discuss and select the optimal therapeutic and diagnostic management.
Мировой опыт оказания медицинской помощи пациентам с травмой демонстрирует высокую эффективность применения телемедицины в организации оказания медицинской помощи и эффективном и адекватном осуществлении лечебных и диагностических мероприятий. Состояние системы здравоохранения Украины не позволяет в полной мере проводить диагностические мероприятия и оказывать медицинскую помощь во всех медицинских учреждениях страны. Таким образом, есть спрос на консультирование практикующих врачей по вопросам проведения контроля повреждений, динамики лечения, а также на предоставление возможности обсуждения и выбора оптимального менеджмента лечения и диагностики.
Світовий досвід надання медичної допомоги пацієнтам із травмою демонструє високу ефективність застосування телемедицини в організації надання медичної допомоги й ефективному й адекватному здійсненні лікувальних та діагностичних заходів. Стан системи охорони здоров’я України не дозволяє повною мірою проводити діагностичні заходи й надавати медичну допомогу у всіх медичних закладах країни. Таким чином, є попит на консультування практикуючих лікарів із питань проведення контролю пошкоджень, динаміки лікування, а також на надання можливості обговорення й вибору оптимального менеджменту лікування й діагностики.
Статья опубликована на с. 45-47
World experience of care to trauma victims demonstrates the high efficiency of the methods of telemedicine in the organization of care to trauma victims, and effective and adequate implementation of therapeutic and diagnostic activities.
The actual conditions of the health system of Ukraine does not allow for a full medical diagnostic aid all medical institutions of Ukraine.
There is therefore a need for constant consultation practitioners majoring in damage control dynamics of treatment, as well as providing opportunities to discuss and select the optimal therapeutic and diagnostic activities.
The increase in the number of severity and types of injuries leads to the necessity of highly skilled, highly specialized and high–tech medical care for patients with polytrauma.
World experience providing medical care to victims of trauma indicates high efficiency of telemedicine methods in the organization of medical care to victims of trauma effective and adequate implementation of therapeutic and diagnostic measures (Vladzimirskyy A.V., 2009–2010).
In fact, the current situation of the health system of Ukraine does not allow for a full medical and diagnostic care in all medical institutions of Ukraine. Therefore there is a need constant counseling practitioners with specialty in damage control dynamics of treatment and enable discussion and selection of optimal therapeutic and diagnostic measures. The above is only possible when using telemedicine techniques, that ensure interoperability of health care institutions at various levels.
Materials and Methods
We made some analysing of the necessity of the telemedicine consultation and control in 1150 patients with multisystem injuries which assisted in the medical institutions of the second level 1000, and the third level 150 victims.
We studied the necessity for assistance in the diagnosis, to provide recommendations for treatment, and dynamic control.
Also held prognostic study of the effectiveness of telemedicine activities in 110 patients, referring promotion of such measures to improve the survival of victims.
All calculations were conducted in accordance with the criteria and requirements of evidence–based medicine by using computer technology, that all the provisions and findings are within probabilities.
Results and discussion
The study found that the advice actually require 82 % of the victims who was given medical treatment in medical institutions of the second level, and 36 % of victims who received assistance in third level institutions.
Needs analysis uses of telemedicine technology in providing assistance to victims are treated as second–tier institutions.
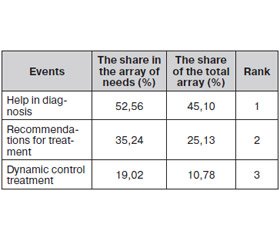
These results are shown in Table 1.
/46/46.jpg)
As seen from Table 1 caused the greatest need for effective measures in terms of diagnosis and adequate. Thus, 52.56 % array advice, or 45.10 % of the total array. Advisory services to provide recommendations on treatment of victims is in the second level of 35.24 %, and advice or 25.13 % of the array. Additional help for the dynamic control is 19.02 % or 10.78 % of the total array and is ranked in third place. Thus, it should be noted that the main problem that can be solved by consultation with highly qualified specia–lists in the field of injury problems of diagnosis.
Recommendations for treatment are necessary rate 1.5 times less, and in a dynamic control 2.7 times less
These patients needed specialist call bet the second level, which led to the detention of adequate medical assistance to 189 minutes. Expert analysis of cases showed that the vast majority of aid could be accelerated and made using telemedicine technology.
Analysis of the data presented in Table 2 indicate that the vast majority of consultative and diagnostic assistance could be provided via telemedicine technology. Most in determining treatments and diagnostics 74.05, 68.74 %. Overall, 72.32 % of the additional needs advice in the course of providing emergency medical care were treated as second–tier institutions can be resolved telemedicine methods, with an average expected lifetime reaches 18 minutes, which is 10 times less. In studying the need for advisory assistance in third level institutions found that this required only 20.06 % while the distribution of aid given in Table 3.
As seen from Table 3, the structure needs to conduct additional measures Level 3 is other than establishments 2nd level.
First, only 20.06 % need additional advice, secondly first is the need for consultative assistance for the treatment of victims who make up 90.32 % or 18.67 % of the array.
Diagnostic measures constitute only 35.48 % of the array needs or 7,33 % of the array.
Dynamic control treatment needed 19,35 % panels needs, or 4 % of the array.
While telemedicine techniques can be applied to a limited extent. As the data set forth in Table 4, the use of telemedicine technology as methods to perform additional advice is only 20 %, while most substitution necessary in the diagnosis of injuries. As proven analysis of cases of damage — this is due to the most severe and difficult to diagnosis damage. This assistance was needed for therapeutic measures half. That there is a real need for consultant call the third level. So the analysis indicates that the use of telemedicine technology is most appropriate in health care institutions second level. The use of telemedicine technology to provide health care, organization and implementation of therapeutic and diagnostic measures in 110 patients with polytrauma who were given medical care in second level institutions has proven that expert estimated figures fully confirmed. The use of telemedicine technology enhanced the survival of victims to 14.55 % due to the improvement of the quality of diagnosis, optimizing the volume and characteristics of therapeutic techniques, reduction of clinical decision–organizational solutions for conducting Clinical Diagnostic measures.
Conclusions
1. The use of telemedicine technology in the process of care in patients with polytravma appropriate in medical institutions of the second level.
2. There is a difference between need and feasibility of telemedicine technology in institutions 2nd and 3rd level, with the second level there is a need for treatment guidelines at the third level diagnostics.
3. The use of telemedicine technology can increase the survival of affected 14.5 % by optimizing the provision of emergency medical care.
1. Loane M.A. A comparison of real time and store and for ward teledermatology: a cost benefit study / Loane M.A., Bloomer S.E., Corbett R. [et al.] // Br. J. Dermatol. — 2000. — Vol. 143. — P. 1241–1247.
2. Мінцер О.П. Модель покращення доступності та якості медичної допомоги сільському населенню із застосуванням телемедичних технологій: Методичні рекомендації / Мінцер О.П., Царенко А.В., Матюха Л.Ф. [та ін.]. — К., 2012. — 26 с.
3. Better, Sooner, More Convenient’ Primary Health Care. New Zealand Ministry of Health, Primary Health Care. n.d. [Электронный ресурс] / Режим доступа: http://www.moh.govt.nz/moh.nsf/indexmh/phcs–bsmc
4. Krupinski E. Telemedicine versus in–person dermatology referrals: an analysis of case complexity / Krupinski E., Barker G., Rodriguez G. [et al.] // Telemed. J. — 2002. — Vol. 8. — P. 143–147.
5. Попченко Т.П. Щодо поточного стану та подальших напрямів реформи фінансування та управління системи охорони здоров’я в Україні. Аналітична записка Національного інституту стратегічних досліджень при Президентові України, 2012 / Попченко Т.П. [Електронний ресурс] / Режим доступу: http://www.niss.gov.ua/articles/717

/46/46_2.jpg)